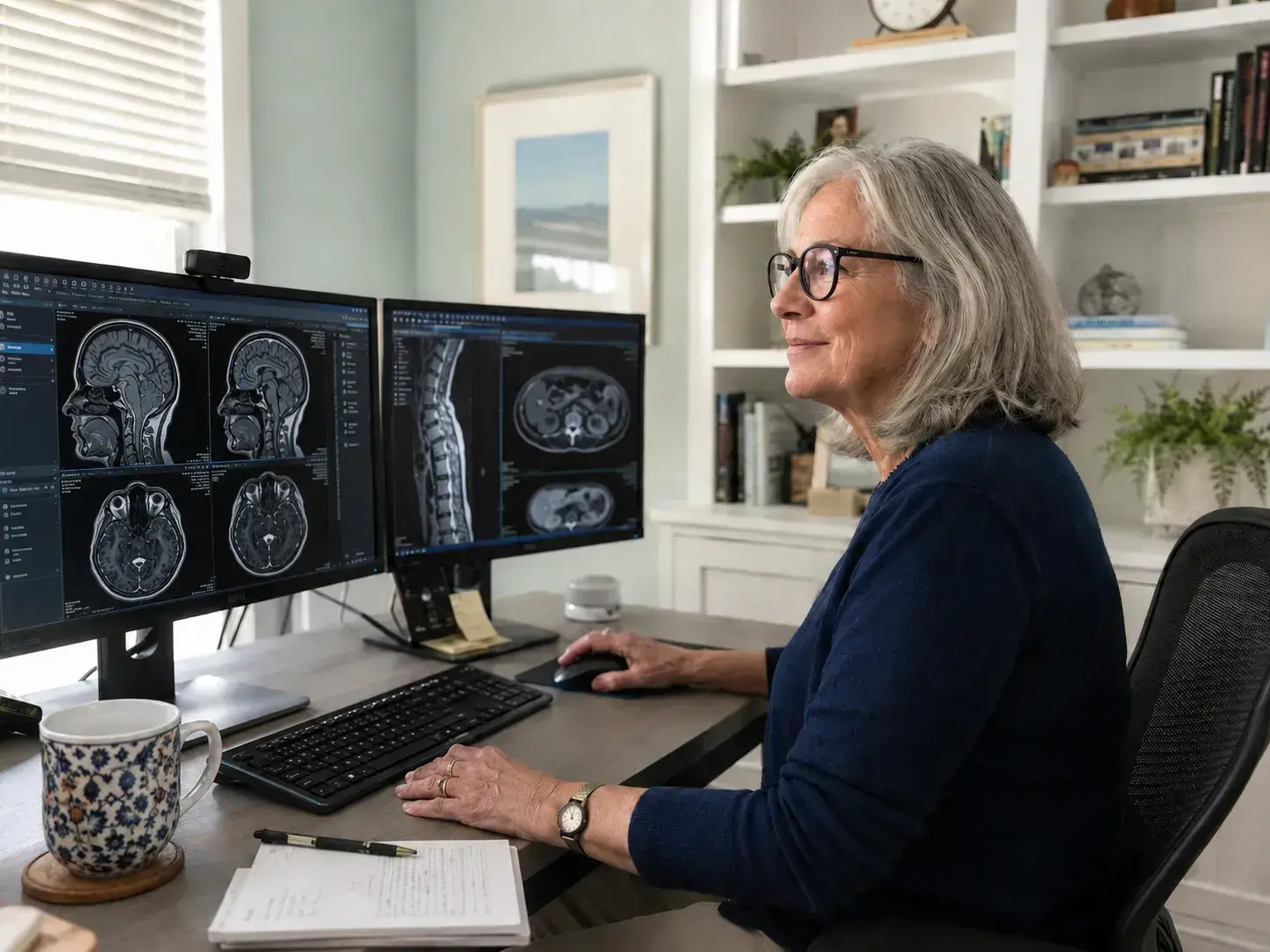
The field of diagnostic imaging is undergoing a profound transformation.
As healthcare demand continues to rise and imaging technology becomes more deeply embedded in everyday clinical care, the traditional hospital reading room is no longer the sole centre of a radiologist’s career.
Today, teleradiology has become a core pillar of modern medical infrastructure. It is no longer simply an after-hours contingency solution. Teleradiology is a dynamic, highly flexible, and increasingly rewarding career path.
Teleradiology is also helping to support the evolving needs of the Australian healthcare system.
If you're a FRANZCR radiologist exploring new ways to structure your work, our guide explains how teleradiology works, the forces driving its rapid growth, and why teleradiology represents one of the most sustainable pathways in modern radiology.
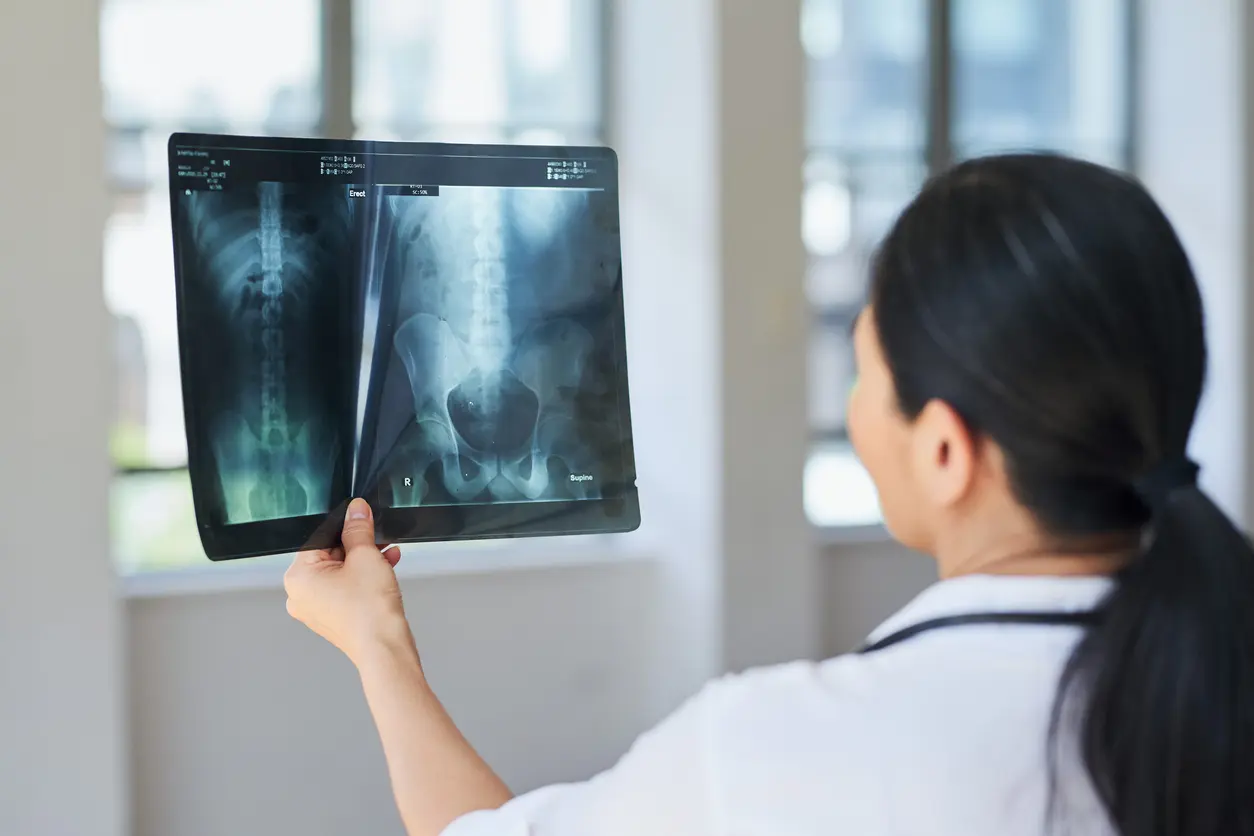
1. What Is Teleradiology and How Does It Work?
Teleradiology is the secure electronic transmission of medical images, such as X-rays, CT scans, MRIs, Ultrasounds and PET scans, from a clinic or hospital to a radiologist who interprets them remotely. The radiologist performs the same diagnostic role as they would on-site, but from a dedicated reporting workstation located at home or another approved domestic location.
The Technological Backbone
Modern teleradiology reporting relies on a highly reliable and secure technology ecosystem designed to replicate, and in many cases enhance, the traditional reading environment.
- PACS (Picture Archiving and Communication System): The central system where imaging studies are stored, accessed and transmitted securely.
- DICOM and HL7 standards: International protocols that ensure imaging data and patient information can be shared seamlessly between healthcare systems.
- Diagnostic workstations: Radiologists use calibrated, multi-monitor setups designed specifically for diagnostic accuracy. These monitors comply with strict clinical standards for image clarity and consistency.
- Secure network infrastructure: Encrypted connections help ensure patient data remains confidential and compliant with Australian healthcare privacy regulations.
In practical terms, the workflow is straightforward:
- A patient undergoes imaging at a clinic.
- Images are uploaded to a secure system.
- A radiologist reviews and reports remotely.
- The referring clinician receives the results promptly.
From the clinician’s perspective, the process is seamless. From the radiologist’s perspective, it offers significantly more flexibility in how and where work is performed.
2. Why Teleradiology Matters in Australia
Australia’s healthcare system is experiencing sustained growth in demand for diagnostic imaging. According to the Australian Institute of Health and Welfare:
- Nearly 2 in 5 Australians receive Medicare-subsidised diagnostic imaging each year.
- More than 27 million diagnostic imaging services are delivered annually.
- MRI volumes have more than doubled over the past decade.
At the same time, the radiology workforce has not expanded at the same rate as imaging demand. This mismatch creates pressure across the healthcare system, particularly in regional and rural communities, high-volume outpatient clinics, after-hours services and subspecialty reporting.
Teleradiology plays an important role in addressing this demand by allowing radiologists to work efficiently across multiple locations without being physically present at each site. Teleradiology supports faster turnaround times, improved patient access to care, more sustainable workloads and better use of specialist expertise. Most importantly, it allows radiologists to continue delivering high-quality patient care while working in a more manageable environment. Teleradiology is not intended to replace traditional radiology practice, but to extend the reach and flexibility of diagnostic services within the broader healthcare system.
3. The Growing Demand for Radiologists and the Opportunity Ahead
Demand for diagnostic imaging continues to rise steadily across Australia. Drivers of this growth include:
- an ageing population
- increased use of advanced imaging technologies
- greater reliance on imaging in routine medical care
- expanded screening programs
- higher patient expectations for timely diagnosis
Healthcare providers are responding by expanding imaging capacity, but workforce supply remains constrained. This creates a clear and sustained demand for experienced radiologists. Teleradiology is increasingly recognised as one of the most effective ways to support this demand while maintaining high clinical standards. For radiologists, this trend represents a significant professional opportunity to work across multiple facilities, choose flexible reporting schedules, maintain consistent case flow and build a sustainable long-term career. Most radiologists today work across a mix of clinical environments, and teleradiology has become an increasingly common component of modern radiology practice.
4. How Teleradiology Fits Within the Broader Radiology System
Teleradiology operates alongside traditional radiology services rather than replacing them. Clinics, hospitals and imaging providers remain central to patient care, while remote reporting helps extend capacity and improve service continuity.
Many radiologists combine on-site clinical work with remote reporting sessions, allowing healthcare providers to maintain consistent service levels while giving doctors greater flexibility in how they practise. In this sense, teleradiology is best understood as part of a broader, integrated radiology model.
5. Who Is Teleradiology Ideal For?
Teleradiology appeals to a wide range of radiologists at different stages of their careers. Common scenarios include:
- Radiologists seeking better work-life balance.
- Parents returning to practice after time away.
- Experienced radiologists wanting more control over their schedules.
- Radiologists living outside major metropolitan centres.
- Practitioners wanting additional reporting sessions alongside existing roles.
- Radiologists approaching later career stages who want to continue working flexibly.
In each of these situations, teleradiology provides a practical and sustainable alternative within the profession.
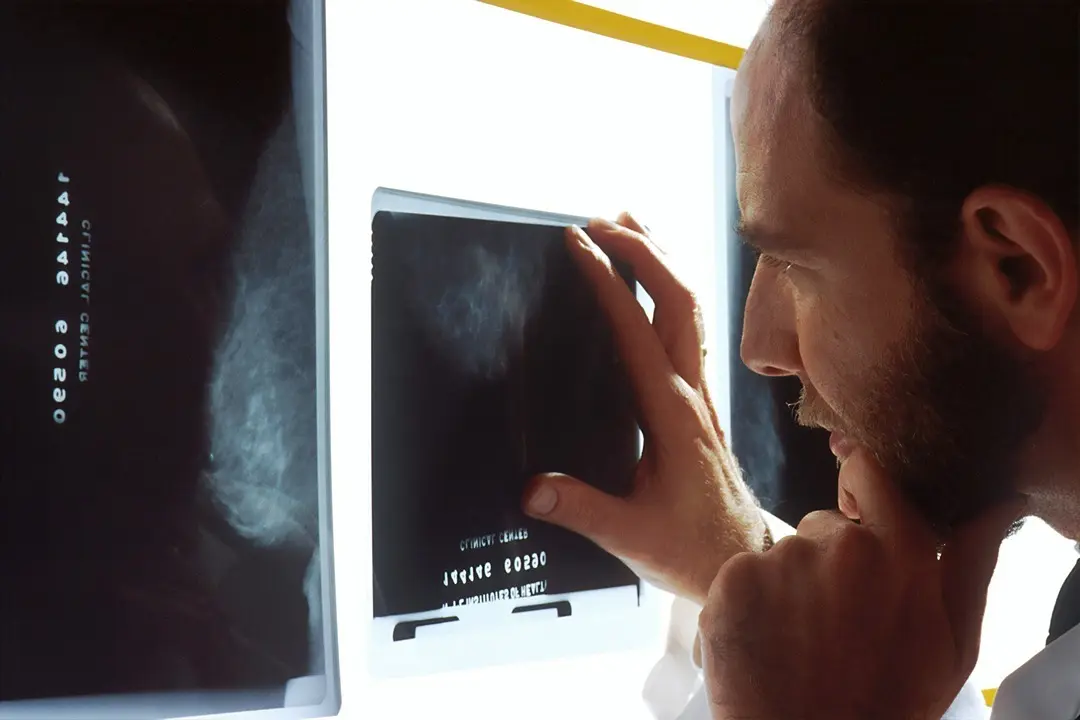
6. A Typical Day in Teleradiology
One of the most common questions radiologists ask is: What does a normal working day actually look like?
In reality, the workflow is familiar and highly structured. A typical reporting session may involve:
- logging into a secure reporting system
- reviewing the assigned worklist
- interpreting imaging studies
- dictating or voice-recognising reports
- submitting completed reports electronically and consulting with colleagues when required
The key difference is the environment. Instead of commuting to a hospital or clinic, teleradiologists can work from a dedicated home workstation designed specifically for diagnostic reporting. This often results in fewer interruptions, greater concentration, more efficient reporting, reduced fatigue and improved work-life balance.
7. Common Modalities and Case Mix in Teleradiology
Teleradiology encompasses a wide range of imaging modalities, including X-ray, CT, MRI, ultrasound, musculoskeletal imaging, general diagnostic imaging and emergency or after-hours reporting. The exact case mix varies depending on the provider and clinical setting, but reputable teleradiology services typically maintain consistent reporting volumes, predictable workflows and a balanced case distribution that helps keep a radiologist’s skill set sharp.
8. The Professional Benefits of a Teleradiology Career
When supported by well-structured systems and experienced providers, teleradiology can reduce many of the operational pressures associated with traditional practice.
Work-Life Flexibility
One of the most significant advantages is the ability to control when and how work is performed. Teleradiologists can choose their own reporting hours, work part-time or full-time, take on additional sessions when desired and schedule work around family or personal commitments. Many radiologists find that flexible reporting arrangements allow them to remain in the workforce longer while supporting long-term career sustainability.
Geographic Freedom
Teleradiology allows radiologists to live where they prefer while maintaining access to high-quality clinical work, whether that is in regional locations, coastal communities, lifestyle-focused areas or urban settings.
Competitive and Transparent Remuneration
Income often reflects reporting activity. Additional sessions can increase earnings, and workload can be scaled up or down as needed. Independent teleradiology networks may also offer transparent compensation models that give radiologists a clearer understanding of how their work is structured and rewarded.
A Focused Working Environment
Working remotely can support improved concentration, greater reporting efficiency, reduced stress and, ultimately, better professional satisfaction.
9. Quality, Safety and Clinical Standards in Teleradiology
A common misconception is that remote reporting compromises clinical rigour. In reality, Australian teleradiology is governed by strict regulatory frameworks designed to support patient safety and diagnostic accuracy. To report on domestic cases and bill Medicare, a teleradiologist must hold a Fellowship of the Royal Australian and New Zealand College of Radiologists (FRANZCR) and maintain a valid Australian Medicare Provider Number. It is also worth noting that, for Medicare compliance, the reporting radiologist must be physically located in Australia both at the time the scan is performed and at the time they report the case. This helps ensure that remote reporting meets the same specialist standards as on-site hospital reporting.
At an operational level, reputable teleradiology requires:
- Diagnostic-grade monitors: Ensuring high-resolution clarity that meets GSDF calibration standards.
- Secure data transmission: Protecting patient privacy through end-to-end encryption.
- Structured reporting systems: Delivering clear, standardised insights to referring physicians.
- Clinical governance processes: Maintaining accountability and transparency in remote operations.
- Peer review and quality assurance programs: Supporting a culture of continuous clinical improvement and collaboration among remote peers.
10. Long-Term Career Pathways in Teleradiology
Teleradiology careers are no longer just a temporary stepping stone. For many radiologists, it has become a meaningful long-term career pathway. Sustainability, however, depends heavily on the systems, support and professional culture surrounding the role.
A sustainable teleradiology career can offer:
- Professional stability: Supported by strong relationships with established clinical networks.
- Predictable workload: Helping radiologists manage reporting volumes more sustainably.
- Ongoing clinical engagement: Encouraging continued learning and subspecialty development.
- Career longevity: Providing a flexible model that can adapt to changing personal and professional priorities over time.
11. Support and Infrastructure: What Radiologists Can Expect
Working remotely should never mean working in isolation. The success of a teleradiologist relies heavily on the technical and administrative backbone supporting them. Leading providers invest heavily in making sure radiologists can focus on clinical work rather than operational friction.
Radiologists can expect:
- Diagnostic workstations: Provided and configured for efficient reporting.
- Secure reporting software: Including state-of-the-art voice recognition and PACS integration.
- Technical setup assistance: Practical support in creating a clinical-grade reporting space at home.
- Ongoing IT support: Dedicated technical help to resolve workflow issues promptly.
- Administrative coordination: Professional support to help manage credentialling, provider numbers and clinical liaison requirements.
12. Conclusion - A More Flexible and Rewarding Path Forward
Teleradiology represents a natural evolution in the practice of diagnostic imaging. It allows radiologists to deliver high-quality patient care while working in a more flexible, efficient and technologically advanced environment. For many professionals, it provides the opportunity to reclaim control over their schedule, maintain a strong clinical focus, achieve better work-life balance and build a sustainable long-term career. As demand for imaging continues to grow across Australia, teleradiology will remain an important part of the radiology landscape, supporting a model of care that benefits both patients and practitioners.
Explore Radiology Careers at PRO Radiology or contact our team directly at recruitment@proxraymanagement.com.
References & Further Reading
- Grand View Research: Teleradiology Market Size & Share Industry Report, 2025-2030
- Australian Institute of Health and Welfare (AIHW): Pathology, imaging and other diagnostic services
- National Institutes of Health (NCBI): The Growing Problem of Radiologist Shortages: Australia and New Zealand's Perspective
- Radiological Society of North America (RSNA): Finding Cures for Radiologist Burnout
- PRO Radiology FAQs: Work Structure, Flexibility, and Income Details
Frequently Asked Questions About Teleradiology
Can Australian teleradiologists work from anywhere?
Yes, but with strict regulatory and technical caveats. From a lifestyle perspective, a radiologist can set up their reporting workstation in a regional town, a coastal community, or an urban centre. However, the legal boundaries are rigid. To legally issue final reports and bill the Australian government, a teleradiologist must hold a Fellowship of the Royal Australian and New Zealand College of Radiologists (FRANZCR) and maintain an active Australian Medicare Provider Number. It is also worth noting that, for Medicare compliance, the reporting radiologist must be physically located in Australia both at the time the scan is performed and at the time they report the case. As long as these credentials are met, and the reporting location has the necessary secure internet infrastructure and calibrated monitors, the radiologist enjoys significant geographic flexibility within Australia.
What technical infrastructure is required to report from home?
Modern remote reporting requires a robust, clinical-grade technology stack that mirrors—or exceeds—the setup found in a traditional hospital reading room. A standard domestic setup typically requires:
- Diagnostic-Grade Workstations: Multi-monitor setups (often 3MP to 5MP displays) specifically designed for medical imaging.
- GSDF Calibration: Strict adherence to the Grayscale Standard Display Function. Monitors must undergo regular software calibration to ensure image luminance and contrast do not drift, guaranteeing diagnostic precision.
- Secure Network Redundancy: High-speed, enterprise-encrypted internet connections (often with a backup failover) to handle massive DICOM files without latency.
- Integrated Software: Advanced PACS, voice-recognition dictation software, and secure communication portals.
How do remote radiologists maintain clinical context without being on-site?
One of the biggest historical frustrations with remote reporting was receiving a complex scan with a one-word clinical indication like "pain." Today, premium teleradiology networks solve this through deep systems integration. By utilizing HL7 protocols, advanced teleradiology platforms integrate directly with a clinic's Electronic Medical Record (EMR) system. This ensures the remote radiologist has immediate access to the patient's comprehensive medical history, digitized request forms, previous imaging studies, and detailed clinical notes. Furthermore, high-quality providers maintain direct, secure communication channels (such as instant chat or priority phone lines) so the remote radiologist can instantly confer with the referring physician or the on-site radiographer.
Does teleradiology replace the need for on-site radiologists?
Absolutely not. Teleradiology is designed to complement and support on-site radiology departments, acting as an elastic extension of the local team. It is a highly effective solution for managing out-patient reporting backlogs, clearing emergency department queues, and handling routine overflow. By outsourcing these high-volume tasks, on-site radiologists are freed up to focus on the clinical work that requires a physical presence, such as ultrasound-guided injections, biopsies, fluoroscopy, and participating in complex Multidisciplinary Team (MDT) meetings.
Are teleradiology reports considered preliminary or final?
In the early days of the industry, "nighthawk" teleradiology services often provided preliminary (or "wet") reads that required an on-site doctor to over-read and finalise the next morning. Today, the standard has shifted entirely. In the Australian out-patient and private practice context, teleradiologists provide final, actionable diagnostic reports. Because the remote reporting doctors hold the exact same FRANZCR specialist qualifications as hospital-based doctors, their reports are definitive. This allows referring GPs and specialists to make immediate, confident treatment decisions without waiting 24 hours for a secondary review.
How does teleradiology ensure patient data privacy?
The transmission of medical images across domestic networks relies on enterprise-grade cybersecurity to adhere to the strict mandates of the Australian Privacy Act 1988. Patient data is protected through several layers of security:
- End-to-End Encryption: DICOM images and HL7 text data are encrypted both in transit (via Virtual Private Networks) and at rest.
- Zero-Footprint Viewers: Patient images are viewed securely through the platform but are never permanently downloaded or stored on the radiologist's local home hard drive.
- Access Controls: Strict identity verification, multi-factor authentication (MFA), and comprehensive audit trails ensure that only authorised clinicians can view a patient's file.
How are remote radiologists typically compensated?
Remuneration in teleradiology is highly transparent, highly competitive, and generally tied directly to reporting output rather than a fixed hourly salary. Most networks use a per-case or output-based structure (often tied to the complexity of the modality), which directly rewards a radiologist's efficiency and speed. The major differentiator lies in the corporate structure of the provider. While large, private-equity-backed firms may cap earning potential, independent out-patient providers often offer more lucrative fee-splits and unique incentives—such as equity participation plans—allowing dedicated radiologists to benefit directly from the long-term growth of the business.